Facing a heart valve problem can be one of the most unsettling experiences of a patient’s life. When a cardiologist recommends Balloon Valvuloplasty, one of the first questions that comes to mind is: “Is this major surgery?” The fear of open-chest operations, prolonged hospital stays, and lengthy recovery periods is entirely understandable. Fortunately, the answer may be more reassuring than you expect.
Unlike traditional open-heart surgery, it does not require cutting open the chest or stopping the heart. Instead, a thin, flexible tube called a catheter is threaded through a blood vessel to reach the affected valve, where a small balloon is inflated to widen the narrowed opening.
What Is Balloon Valvuloplasty?
Balloon Valvuloplasty is a non-surgical, catheter-based cardiac procedure used to treat heart valve stenosis, a condition where one or more heart valves become abnormally narrow, restricting blood flow through the heart. It is performed in a cardiac catheterization laboratory (cath lab) and is considered part of interventional cardiology.
Conditions Treated
The procedure is most commonly used to treat the following valve conditions:
- Mitral Valve Stenosis: Narrowing of the mitral valve, which sits between the left atrium and left ventricle. This is the most common indication for balloon valvuloplasty, particularly in patients with rheumatic heart disease.
- Aortic Valve Stenosis: Narrowing of the aortic valve, often seen in older adults due to calcium buildup. Balloon valvuloplasty in this case may be used as a temporary or palliative measure.
- Pulmonary Valve Stenosis: Narrowing of the pulmonary valve, a condition more frequently encountered in children and young adults, often congenital in origin. Balloon valvuloplasty is often the preferred treatment in these cases.
How the Procedure Works
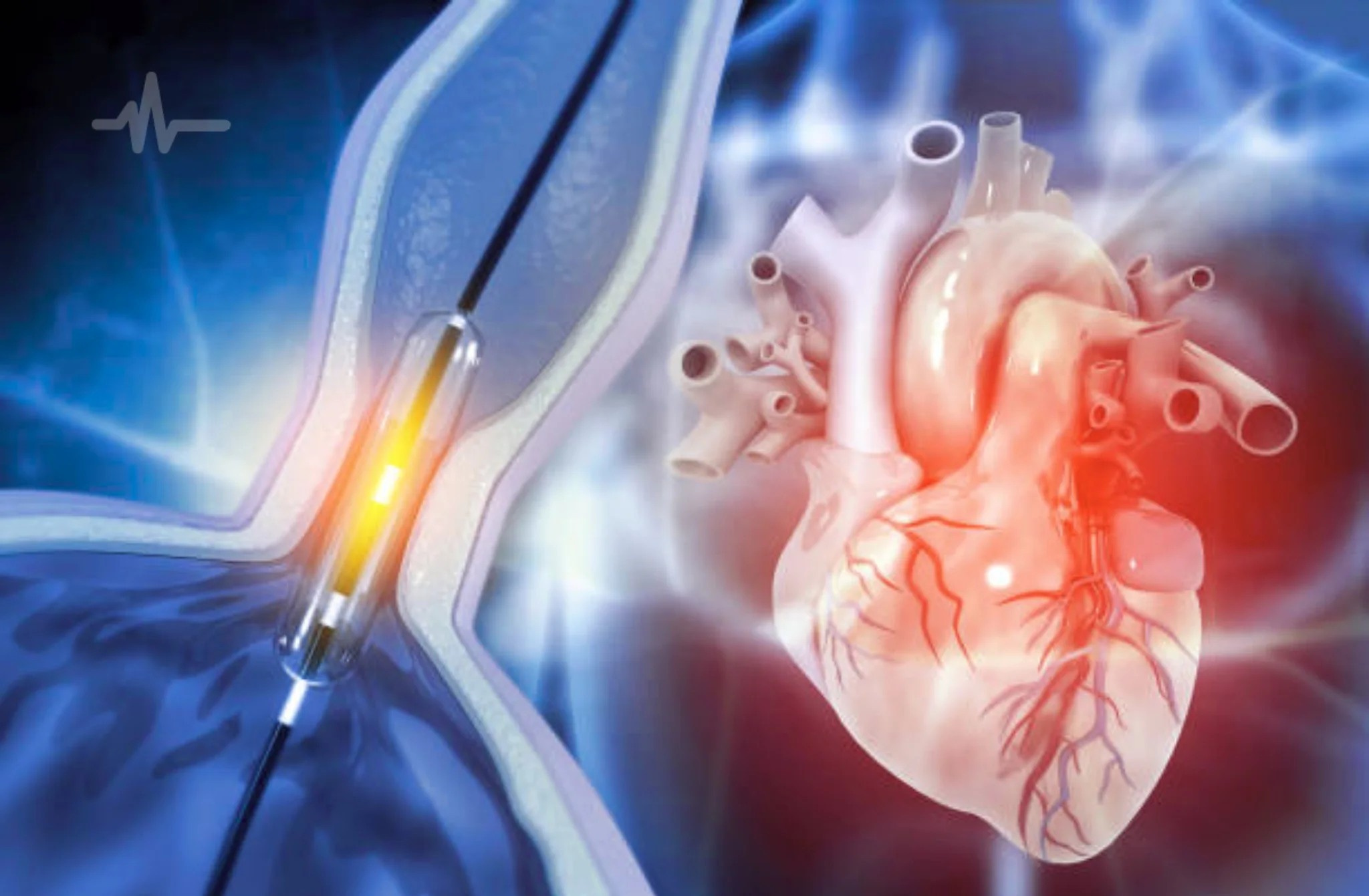
A catheter (a long, thin, flexible tube) is inserted into a blood vessel, usually in the groin or wrist, and guided through the body to the heart using real-time X-ray imaging called fluoroscopy. Once the catheter reaches the affected valve, a deflated balloon at its tip is carefully positioned within the narrowed valve opening.
The balloon is then inflated for a few seconds to mechanically separate the fused or thickened valve leaflets, widening the valve opening and allowing blood to flow more freely. The balloon is then deflated and removed. Crucially, this is achieved without removing or replacing the valve, making it far less invasive than surgical valve repair or replacement. The result is improved blood flow, reduced pressure on the heart, and significant symptom relief in most patients.
Is Balloon Valvuloplasty a Major Surgery?
No, Balloon Valvuloplasty is not considered major surgery. However, it is a serious cardiac procedure that carries its own set of risks and must be performed by skilled interventional cardiologists.
Balloon Valvuloplasty is fundamentally different. Here is why it is not classified as major surgery:
- No chest incisions or sternotomy required
- No cardiopulmonary bypass (heart-lung machine) is used
- Performed under local anesthesia with sedation, not general anesthesia, in most cases
- The heart continues to beat normally throughout the procedure
- Recovery is measured in days, not weeks or months
- It is performed through a small puncture in a blood vessel, not a surgical cut
That said, it would be a mistake to minimize its seriousness. The heart is involved, and any cardiac procedure carries inherent risks. The balloon valvuloplasty sits in a very different category from traditional open-heart surgery, one that is substantially less invasive and generally safer for appropriate candidates.
Is Balloon Valvuloplasty Minimally Invasive?
Yes, Balloon Valvuloplasty is unequivocally classified as a minimally invasive cardiac procedure. Understanding what this means helps patients set appropriate expectations for the procedure and recovery.
Minimally Invasive
A minimally invasive procedure is one that accesses the target area through small punctures, natural openings, or tiny incisions rather than large surgical cuts. In the context of cardiology, it refers to catheter-based interventions that avoid opening the chest.
Advantages of the Minimally Invasive Approach
- No sternotomy (chest bone is never cut or opened)
- Only a small needle puncture in the skin, typically at the groin or wrist
- Significantly reduced blood loss compared to open surgery
- Much shorter hospital stay, typically 24 to 48 hours
- Faster return to daily activities and work
- Lower risk of infection at the surgical site
- Less postoperative pain and discomfort
Balloon Valvuloplasty Procedure: Step-by-Step
Pre-Procedure Preparation
Before the procedure, the medical team conducts a thorough evaluation to ensure safety and suitability. This typically includes:
- Blood tests (complete blood count, coagulation profile, kidney function)
- Echocardiogram to assess valve anatomy and function
- Electrocardiogram (ECG) to evaluate heart rhythm
- Chest X-ray and cardiac CT or MRI in some cases
- Review of all current medications, some blood thinners may be paused
- Fasting for 4–8 hours prior to the procedure
- Consent discussion covering risks, benefits, and alternatives
Patients are asked to arrive at the hospital several hours before the procedure. A nurse will insert an intravenous (IV) line, shave and clean the access site (usually the groin), and apply monitoring electrodes.
The Procedure: Step by Step
The entire procedure typically takes 1 to 2 hours. Patients are then transferred to a monitored recovery area or cardiac care unit for observation.
1. Anesthesia: A local anesthetic is injected at the access site (groin or wrist) to numb the area. Intravenous sedation is given to help the patient relax. Most patients are awake but drowsy throughout.
2. Arterial/Venous Access: A small needle punctures the femoral vein or artery in the groin (or the radial artery at the wrist). A sheath (plastic tube) is inserted to maintain access.
3. Catheter Navigation: A guidewire is threaded through the sheath and advanced toward the heart under fluoroscopic (real-time X-ray) guidance. The catheter follows along the guidewire.
4. Transseptal Puncture (if needed for mitral valve): For mitral valve procedures, the cardiologist may puncture the septum (wall between the heart’s two upper chambers) to access the left side of the heart.
5. Balloon Positioning: The balloon catheter is carefully positioned at the narrowed valve opening using imaging guidance and pressure measurements.
6. Balloon Inflation: The balloon is rapidly inflated for 3–5 seconds, mechanically stretching open the fused valve leaflets. This may be repeated several times to achieve optimal results.
7. Assessment & Removal: Post-inflation pressure measurements and echocardiography confirm improvement. Catheters and sheaths are removed, and the access site is closed with manual pressure or a closure device.
Balloon Valvuloplasty Recovery Time & Aftercare
Immediate Recovery (First 24–48 Hours)
Following the procedure, patients are monitored closely in a cardiac recovery unit. During this period:
- Vital signs (blood pressure, heart rate, oxygen saturation) are continuously monitored
- The access site is checked regularly for bleeding or hematoma
- Patients are asked to keep the leg straight for several hours if the groin was used
- Pain at the puncture site is usually mild and manageable with over-the-counter analgesics
- Oral fluids are reintroduced once the patient is alert and stable
Most patients are discharged within 24 to 48 hours, provided their condition is stable and there are no complications. This stands in sharp contrast to open-heart surgery, which typically requires 5–10 days of hospitalization.
Full Recovery Timeline
| Milestone | Balloon Valvuloplasty | Open-Heart Surgery |
| Hospital discharge | 24–48 hours | 5–10 days |
| Walking normally | 1–2 days | 1–2 weeks |
| Return to light activity | 3–5 days | 4–6 weeks |
| Return to work (desk job) | 1 week | 6–8 weeks |
| Full physical recovery | 1–2 weeks | 2–3 months |
Aftercare Instructions
- Avoid heavy lifting (over 5 kg) for at least one week
- Keep the puncture site clean and dry; watch for signs of infection
- Take all prescribed medications, including anticoagulants, as directed
- Attend all follow-up appointments, usually scheduled at 1 week and 1 month post-procedure
- Report any chest pain, shortness of breath, or unusual swelling immediately
- Adopt heart-healthy lifestyle changes: low-sodium diet, moderate exercise, smoking cessation
Balloon Valvuloplasty Success Rate & Benefits
The success of Balloon Valvuloplasty depends significantly on the type of valve affected, the degree of stenosis, and individual patient factors. If you or a loved one is dealing with valve-related conditions, exploring Valvular Heart Disease Treatment with a specialist can help determine the most suitable approach. Overall, outcomes are favorable for appropriately selected patients.
Success Rates by Valve Type
- Mitral Valve Stenosis: Balloon valvuloplasty (also called percutaneous mitral balloon commissurotomy or PMBC) is highly effective, with technical success rates of 85–95%. Significant symptom improvement is seen in the majority of patients, with 5–10 year event-free survival rates ranging from 50–80% depending on the degree of calcification.
- Pulmonary Valve Stenosis: This is considered the gold-standard treatment in children and young adults with isolated pulmonary valve stenosis. Success rates exceed 90%, with durable long-term results in most patients.
- Aortic Valve Stenosis: Success rates are more modest (50–70%), and the benefits may be short-lived due to restenosis. It is generally used as a palliative treatment or a bridge to surgical or transcatheter aortic valve replacement (TAVR).
Risks and Complications of Balloon Valvuloplasty
While Balloon Valvuloplasty is far less risky than open-heart surgery, it is not without potential complications. Understanding these risks is an important part of informed consent and decision-making.
Common Risks (Minor)
- Bruising, minor bleeding, or hematoma at the catheter insertion site
- Temporary irregular heart rhythms (arrhythmias) during or after the procedure
- Mild fever or inflammatory response in the first 24–48 hours
- Contrast dye reaction (allergic response in sensitive patients)
- Temporary kidney stress from contrast dye was monitored with post-procedure blood tests
Serious Complications (Less Common but Important)
- Significant valve damage or worsening valve regurgitation (blood flowing backwards)
- Stroke or transient ischemic attack (TIA) due to dislodged blood clots or air emboli
- Cardiac tamponade (blood accumulating around the heart) rare but can be life-threatening
- Restenosis (re-narrowing of the valve) more common in aortic valvuloplasty
- Emergency open-heart surgery if a serious complication arises during the procedure
- Heart attack (rare) due to disruption of the coronary blood flow
Factors That Increase Risk
- Advanced age and frailty
- Severe valve calcification or rigidity
- Presence of blood clots in the left atrium (especially in mitral stenosis)
- Existing heart failure or reduced ejection fraction
- Significant comorbidities (diabetes, kidney disease, lung disease)
Balloon Valvuloplasty vs Open-Heart Surgery
| Factor | Balloon Valvuloplasty | Open-Heart Surgery | Clinical Significance |
| Invasiveness | Minimally invasive (catheter | Highly invasive (open chest) | Severity of procedure |
| Anesthesia | Local + sedation (usually) | General anesthesia | Anesthetic risk |
| Hospital Stay | 24–48 hours | 5–10 days | Time away from home |
| Recovery Time | Days to 1 week | 4–8 weeks | Return to normal life |
| Scarring | Small puncture only | Large sternotomy scar | Cosmetic & physical impact |
| Durability | May require repeat procedures | Longer-lasting correction | Long-term effectiveness |
| Risk Level | Lower overall risk | Higher risk, higher reward | Patient safety considerations |
| Ideal Candidate | High-risk/elderly patients | Younger, complex cases | Who benefits most |
Ideal Candidates for Balloon Valvuloplasty
Not every patient with valve stenosis is a suitable candidate for Balloon Valvuloplasty. Careful evaluation by a cardiologist, often supported by an echocardiographer and a multidisciplinary heart team, is essential to determine whether this approach is appropriate.
Ideal Candidates
- Non-calcified mitral/pulmonary stenosis
- Younger patients with pliable valves
- Elderly or high-risk surgical patients
- Temporary relief before valve replacement
- Patients with comorbidities (e.g., kidney disease)
Less Suitable Candidates
- Heavily calcified or rigid valves
- Patients with significant valve regurgitation
- Complex structural heart abnormalities
- Those who failed prior to valvuloplasty
- Patients with blood clots in the heart
Conclusion
For patients facing heart valve stenosis, Balloon Valvuloplasty represents a remarkable advance in cardiac medicine: a way to improve quality of life, restore normal blood flow, and avoid the rigors of open-heart surgery all through a small puncture in the skin. Its minimally invasive nature, short recovery time, and favorable safety profile make it a powerful option for appropriately selected patients, particularly the elderly or those with high surgical risk.
The most important step you can take is to have an open and informed conversation with your cardiologist. Bring your questions, share your concerns, and ask about all available options. At Atlantic Cardiovascular, our team is dedicated to guiding patients through every stage of their cardiac care with expertise, compassion, and a commitment to the best possible outcomes. With the right information and the right medical team, patients with valve stenosis can face the road ahead with clarity and confidence.