If your doctor recommends a mesenteric artery duplex ultrasound, one of your first questions is likely whether insurance will cover it. In most cases, the answer is yes, but only when the exam is considered medically necessary.
Coverage depends on your symptoms, documented diagnosis, insurance plan type, and whether prior authorization is required. Medicare, Medicaid, and most private insurance companies approve the test when ordered to evaluate reduced blood flow in the mesenteric arteries.
What Is a Mesenteric Artery Duplex Ultrasound?
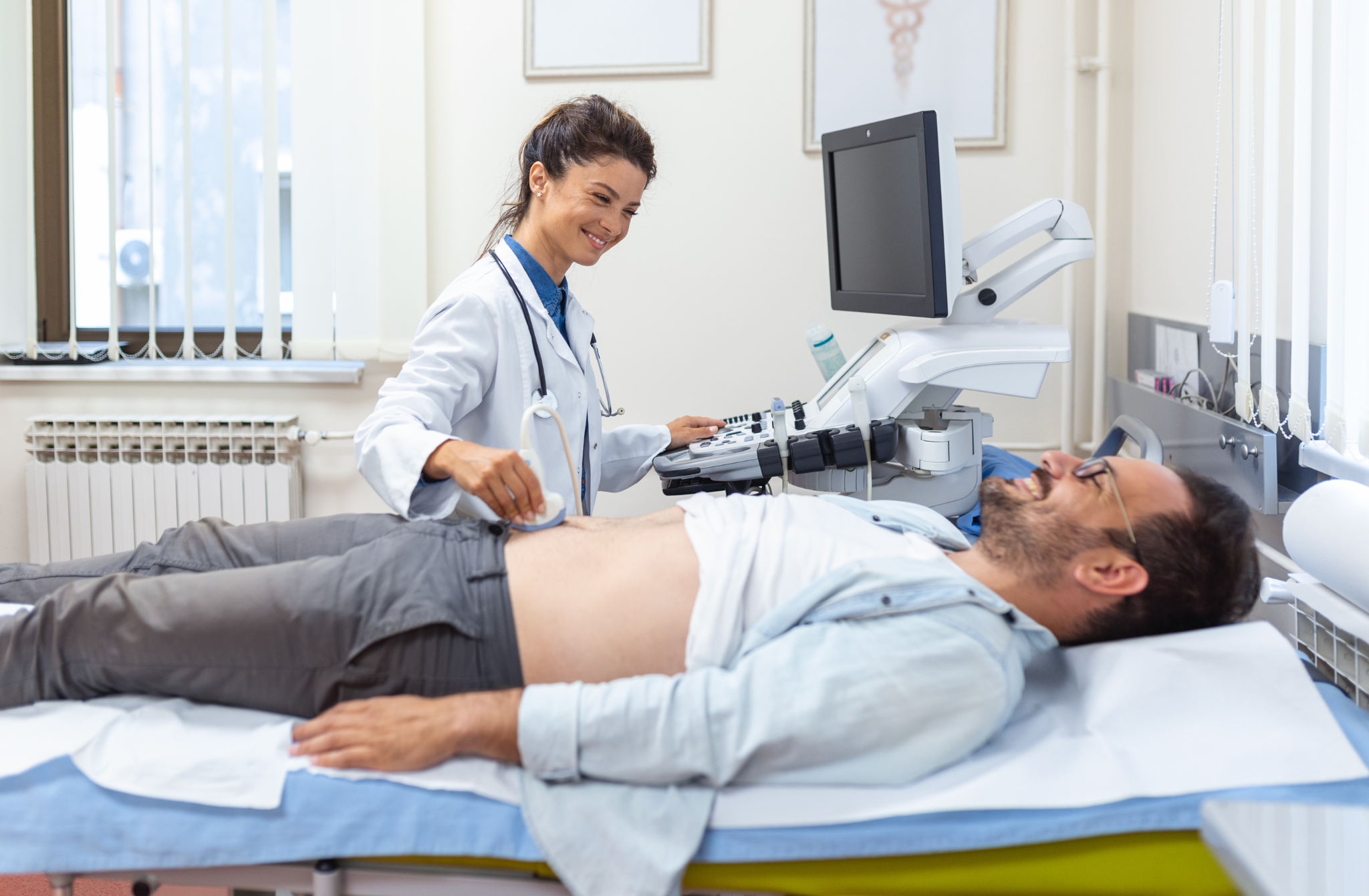
A mesenteric artery duplex ultrasound is a noninvasive vascular imaging test used to check blood flow in the arteries that supply the intestines. The test combines standard ultrasound imaging with Doppler technology to identify:
- Narrowed or blocked arteries (stenosis)
- Reduced or absent blood flow
- Chronic mesenteric ischemia
- Post-procedural changes after stenting or surgery
It is commonly used to evaluate the superior mesenteric artery (SMA), celiac artery, and inferior mesenteric artery (IMA). Unlike CT scans or angiograms, this ultrasound does not use radiation or contrast dye, making it a preferred first-line imaging test for many patients.
When Is the Test Medically Necessary?
Insurance providers only cover diagnostic imaging when there is a documented medical reason for the exam. A mesenteric artery duplex ultrasound is generally considered medically necessary when a patient has one or more of the following:
- Postprandial abdominal pain (pain after eating)
- Unexplained, unintentional weight loss
- Suspected or confirmed chronic mesenteric ischemia
- History of vascular disease (atherosclerosis, aortic disease)
- Mesenteric artery stenosis was found on other imaging
- Follow-up monitoring after mesenteric stenting or bypass surgery
Physicians must document these symptoms clearly in the patient’s medical record before submitting the claim to insurance. Incomplete documentation is one of the leading causes of claim denials.
CPT and ICD-10 Billing Codes
Correct billing codes are essential for insurance approval. Using the wrong CPT or ICD-10 code can result in an automatic denial even when the test is medically appropriate. Verify these codes with your imaging center before your appointment.
CPT Codes (Procedure Codes)
| CPT Code | Description |
| 93975 | Duplex scan of intra-abdominal arteries, complete study, the standard code for mesenteric artery duplex ultrasound |
| 93976 | Duplex scan of intra-abdominal arteries, limited or follow-up study |
| 93971 | Duplex scan of extremity veins (used if lower extremity involvement) |
Common ICD-10 Diagnosis Codes
| ICD-10 Code | Diagnosis |
| K55.1 | Chronic vascular disorders of the intestine |
| K55.0 | Acute vascular disorders of the intestine |
| I77.1 | Stricture of the artery |
| R10.10 | Upper abdominal pain, unspecified |
| R63.4 | Abnormal weight loss |
| Z96.898 | Presence of other specified functional implants (post-stent) |
Does Medicare Cover Mesenteric Artery Duplex Ultrasound?
Yes. Medicare typically covers mesenteric artery duplex ultrasound under Medicare Part B when the test is medically necessary and ordered by a physician.
Medicare Part B
Part B covers outpatient diagnostic services, including vascular ultrasound. Coverage usually applies when:
- A physician orders the test with a documented clinical reason
- Symptoms are clearly recorded in the medical record
- Proper CPT and ICD-10 codes are submitted
- The facility accepts Medicare assignment
Medicare Part B typically pays 80% of the Medicare-approved amount after the annual deductible is met. The patient is responsible for the remaining 20% coinsurance unless they have supplemental (Medigap) coverage.
Medicare Advantage (Part C) Important Differences
If you are enrolled in a Medicare Advantage plan (sometimes called Part C or MA plan), your coverage rules differ significantly from Original Medicare Part B. Medicare Advantage plans are offered by private insurers and must cover at least what Original Medicare covers but they often impose additional requirements such as:
- Prior authorization before imaging is approved
- In-network facility requirements (using an out-of-network vascular lab may result in higher costs or no coverage)
- Referral requirements from your primary care physician
- Step-therapy requirements (requiring a primary care evaluation before specialist referral)
Do Medicaid Plans Cover the Test?
Many Medicaid plans cover mesenteric artery duplex ultrasound, but coverage rules vary significantly by state and by managed care organization (MCO).
In most cases, Medicaid approval depends on:
- Documented medical necessity
- Physician documentation submitted with the prior authorization request
- Referral from a primary care provider or specialist
- Use of an in-network imaging facility
- Prior authorization from the Medicaid managed care plan
Patients should contact their Medicaid plan or managed care organization before scheduling the exam. If you are unsure which number to call, check your Medicaid ID card or the state Medicaid portal for your plan’s contact information.
Is the Test Covered by Private Insurance?
Most private insurance companies cover mesenteric artery duplex ultrasound when it is medically necessary. Common insurers that typically provide coverage include Aetna, Cigna, UnitedHealthcare, Humana, EmblemHealth, Healthfirst, Fidelis, and Oscar, among others.
PPO Plans
PPO plans usually offer the most flexibility. They typically do not require a referral from a primary care physician and allow access to out-of-network providers (though at higher cost). Prior authorization may still be required.
HMO Plans
HMO plans generally require a referral from your primary care physician before specialist imaging is approved. All services must be performed by in-network providers. Using an out-of-network facility usually means zero coverage.
EPO Plans
EPO plans require patients to use in-network providers for all services. They typically do not require referrals for specialists, but prior authorization is commonly required for imaging procedures.
Does the Test Require Prior Authorization?
Yes, many insurance providers require prior authorization before approving a mesenteric artery duplex ultrasound. Prior authorization (sometimes called pre-authorization or pre-approval) is the process by which your insurer confirms that the test is medically necessary before it is performed.
Your physician’s office typically submits the prior authorization request on your behalf. Supporting documentation usually includes:
- Clinical notes documenting symptoms (postprandial pain, weight loss, etc.)
- Relevant diagnosis codes (ICD-10)
- Any prior imaging results or lab findings
- A statement of medical necessity from the ordering physician
- Procedure code(s) being requested (CPT 93975 or 93976)
How to Improve Your Chances of Insurance Approval
There are several practical steps you and your physician can take to reduce the risk of a claim denial.
1. Ensure symptoms are clearly documented in your medical record, including postprandial abdominal pain, unexplained weight loss, or vascular disease history.
2. Verify insurance coverage before scheduling by calling your insurer and asking whether CPT 93975 is covered and whether prior authorization is required.
3. Confirm that the imaging center is in-network for your specific plan.
4. Check that the correct CPT and ICD-10 codes will be submitted, and that they match your documented symptoms.
5. Request written confirmation of prior authorization before your appointment date.
What If Insurance Denies the Claim?
A denial does not necessarily mean the end of the road. Insurance companies are required to give you the opportunity to appeal a denied claim, and many appeals are successful when the right documentation is submitted.
Common Reasons for Denial
- Missing or incomplete prior authorization
- Incorrect CPT or ICD-10 code submitted
- Insufficient documentation of medical necessity
- Out-of-network facility used without prior approval
- The test was considered experimental or not covered under your specific plan
Steps to Appeal a Denied Claim
- Request the denial letter in writing. It must state the specific reason for denial and the applicable policy language.
- Contact your physician’s office to review the denial reason. In many cases, a corrected claim with additional documentation can resolve the issue quickly.
- File an internal appeal with your insurance company. Submit a written appeal letter, the denial letter, your physician’s letter of medical necessity, clinical notes, and any relevant test results or imaging.
- Request a peer-to-peer review if available. This allows your physician to speak directly with the insurance company’s medical reviewer to discuss the clinical rationale.
- File an external appeal if the internal appeal is denied. Patients have the right under federal law (ACA) to request an independent external review. The external reviewer’s decision is binding on the insurer.
- Contact your State Insurance Commissioner if you believe the denial was improper. Most states have a consumer assistance program.
Why This Test Matters
Mesenteric artery disease can restrict blood flow to the intestines and may lead to serious, life-threatening complications if left undiagnosed. A mesenteric artery duplex ultrasound allows physicians to identify vascular problems early without surgery, radiation, or contrast dye exposure.
Early diagnosis may help prevent acute mesenteric ischemia, a condition that can progress rapidly and require emergency intervention. For patients with chronic symptoms, confirming the diagnosis early opens the door to treatment options, including medical management, angioplasty, stenting, or surgical bypass.
Schedule a Mesenteric Artery Duplex Ultrasound
If you are experiencing abdominal pain after eating, unexplained weight loss, or symptoms related to vascular disease, your doctor may recommend a mesenteric artery duplex ultrasound.
Atlantic Cardiovascular provides vascular ultrasound testing and accepts Medicare, Medicaid, and many major insurance plans. Coverage verification and prior authorization assistance may also be available before your appointment.
Medical Disclaimer
This content is for informational purposes only and should not be considered medical, insurance, or financial advice. Coverage for mesenteric artery duplex ultrasound varies by insurance provider, policy terms, medical necessity, and physician documentation. Always consult your doctor and insurance company regarding your specific medical condition and coverage eligibility.