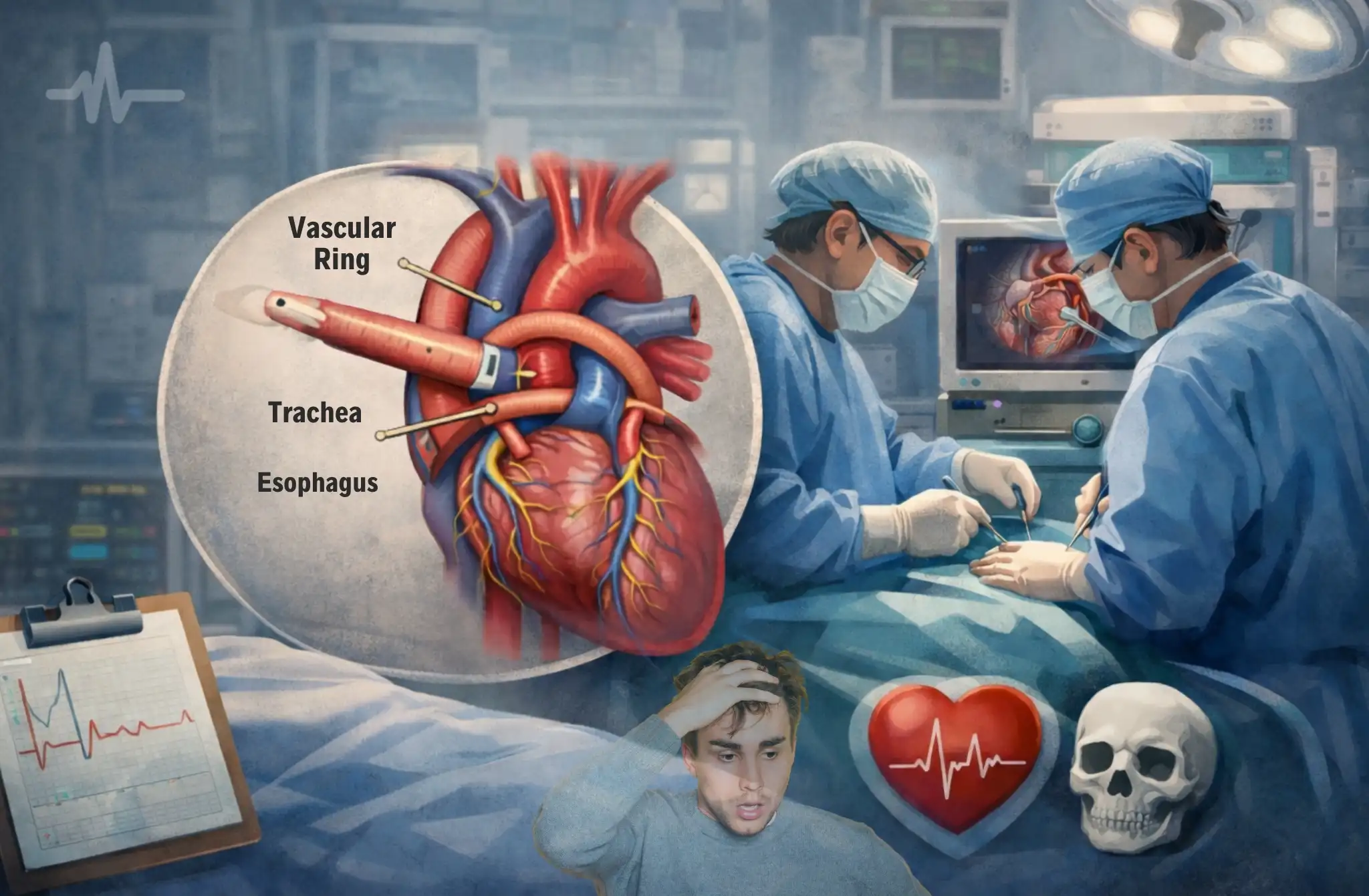
Imagine sitting in a cardiologist’s office, your child on your lap, and hearing the words “vascular ring.” For most parents, those two words trigger an immediate spiral of fear: surgeons, operating rooms, general anesthesia, and a chest opened on the table. The question that dominates everything else is not how the surgery works or what recovery looks like. It is simply: is this dangerous?
A vascular ring is a congenital anomaly in which abnormal blood vessels, typically an abnormal aortic arch arrangement, form a ring that encircles and compresses the trachea, the esophagus, or both. The compression is what causes symptoms: a persistent barking cough, noisy breathing, repeated chest infections, difficulty swallowing, and, in severe cases, life-threatening airway obstruction.
Why Surgery Is Almost Always Necessary
Understanding why surgery is recommended begins with understanding what vascular ring symptoms before surgery actually look like day to day.
The most common presentations include:
- Stridor is a high-pitched, wheezing sound during breathing, especially noticeable during exertion or feeding
- Recurrent respiratory infections, including bronchitis and pneumonia, that keep returning despite treatment
- Chronic cough that does not respond to standard asthma or reflux medications
- Dysphagia: difficulty swallowing solid foods, sometimes described as food getting stuck
- Apnea episodes or cyanotic spells in infants with severe compression
These symptoms do not plateau; they tend to worsen as the child grows, while the vascular structures remain fixed in their abnormal position. Watchful waiting in symptomatic patients is rarely medically sound. The risk of leaving a vascular ring untreated is progressive airway damage, tracheomalacia, recurrent lung infections, and, in worst cases, sudden airway compromise, which almost always outweighs the surgical risk when evaluated properly.
What Happens During Vascular Ring Surgery
One of the most persistent misconceptions about this procedure is that it involves open-heart surgery with a heart-lung bypass machine. For the majority of vascular ring types, this is not the case. Understanding what happens during vascular ring surgery helps dramatically recalibrate the perceived danger level.
The surgery involves identifying the abnormal vascular structure, most commonly a double aortic arch or a right aortic arch with a left ligamentum arteriosum, and dividing the fibrous or vascular band that creates the ring. Once divided, the ring is opened, and the trachea and esophagus are freed from compression. Two main surgical approaches are used:
- Left thoracotomy: A traditional approach through the left side of the chest, used for most double aortic arch cases
- Video-Assisted Thoracoscopic Surgery (VATS) or robotic-assisted: A minimally invasive approach increasingly used at high-volume centers, with smaller incisions, less post-operative pain, and faster recovery.
The procedure is performed under general anesthesia by a pediatric cardiac or thoracic surgeon, typically lasting between one and three hours. Cardiopulmonary bypass is not required in most cases, which removes one of the major risk categories associated with open-heart surgery, a crucial distinction when families are comparing this procedure to other congenital heart surgeries.
How Safe Is Vascular Ring Surgery, Really?
High-volume pediatric cardiac centers report vascular ring surgery success rates exceeding 95 to 98 percent, with vascular ring surgery survival rates approaching 99 percent in elective, non-emergency cases among otherwise healthy patients. Several variables shape the individual risk profile:
- Age at surgery: Younger patients with less cumulative airway damage tend to have better outcomes. Early intervention, before tracheomalacia becomes established, is consistently associated with superior results.
- Type of vascular ring: Double aortic arch, the most common type, carries an excellent prognosis. Rarer forms, such as pulmonary artery sling, carry somewhat higher complexity and risk.
- Presence of associated defects: Some patients have co-existing congenital heart defects. These can increase operative complexity, but surgical planning accounts for them.
- Center volume and surgeon experience: This is arguably the single most important variable. Surgeons and centers performing high volumes of these procedures have significantly lower complication rates than low-volume settings.
Vascular Ring Surgery Risks
No surgery is without risk. An honest discussion of vascular ring surgery risks is essential for informed decision-making. Risks fall into two categories:
Intraoperative Risks
- Bleeding: Division of vascular structures carries an inherent bleeding risk, though this is well-managed in experienced hands
- Anesthesia reaction: Rare but possible, particularly relevant in very young infants
- Recurrent laryngeal nerve injury: The nerve controlling vocal cord function runs near the operative field. Damage can cause hoarseness, though permanent injury is uncommon.
- Incomplete ring division: In rare cases, residual compression may necessitate re-operation
Postoperative Risks
- Chylothorax: Leakage of lymphatic fluid into the chest cavity, requiring drainage and dietary management
- Phrenic nerve injury: Can cause diaphragm paralysis on the affected side
- Pleural effusion or pneumothorax: Fluid or air in the chest cavity, typically managed conservatively
- Wound infection: Low risk with modern sterile technique and prophylactic antibiotics.
These risks, while real, occur in a minority of cases and are manageable at centers with appropriate pediatric surgical infrastructure. The risk-benefit calculation almost universally favors surgical intervention in symptomatic patients.
Vascular Ring Surgery Complications: Short-Term vs. Long-Term
| Short-Term Complications (First 2–4 Weeks) | Long-Term Complications (Months After Surgery) |
| Prolonged Intubation: Some children may need breathing support for a longer period due to airway swelling after surgery. | Tracheomalacia: Softening of the tracheal wall caused by long-term compression before surgery, leading to noisy breathing or mild respiratory symptoms. |
| Feeding Difficulties: Infants may temporarily struggle with swallowing or feeding as the esophagus adapts after pressure from the vascular ring is removed. | Persistent Respiratory Symptoms: Breathing noise or mild airway symptoms may continue for several months while the airway heals and strengthens. |
| Wound-Related Issues: Minor surgical site concerns, such as irritation, redness, or delayed healing, may occur but are usually manageable. | Need for Additional Airway Procedures (Rare): Some children with complex conditions like pulmonary artery sling or complete tracheal rings may require further treatment at specialized centers. |
Vascular Ring Surgery Recovery Time
Vascular ring surgery recovery time varies based on the surgical approach and the patient’s pre-operative condition. A general framework helps families plan effectively:
- Hospital stay: Typically 3 to 7 days for uncomplicated cases. Minimally invasive VATS approaches are often associated with shorter stays of 2 to 3 days.
- First two weeks at home: Activity restrictions apply, no lifting, vigorous play, or sports. Feeding may still require attention in young infants. Pain is generally manageable with oral medications.
- Weeks two to six: Gradual return to normal activity. Breathing improvements typically begin to become noticeable. Follow-up imaging echocardiogram, barium swallow study, or bronchoscopy is scheduled to assess results.
- Three to twelve months: The window during which tracheomalacia-related symptoms gradually improve. Most children show significant or complete resolution within this timeframe.
Families should contact their surgical team promptly if they notice fever, increasing respiratory distress, new cyanosis, or signs of wound infection during recovery. These are the specific red flags that warrant urgent evaluation.
Life After Vascular Ring Surgery
For the vast majority of patients, life after vascular ring surgery is indistinguishable from that of their peers. Long-term follow-up studies consistently show that children who undergo timely vascular ring division go on to lead completely unrestricted lives, participating fully in sports, attending school without limitation, and requiring no ongoing cardiac or pulmonary medications.
The quality-of-life transformation is frequently described by families as dramatic: a child who was repeatedly hospitalized for respiratory infections, struggled to eat, and whose sleep was disrupted by noisy breathing, suddenly able to breathe quietly, eat normally, and develop without the shadow of chronic illness.
Conclusion
So, vascular ring surgery carries real risks, as every surgery does, but it is not inherently dangerous when performed by experienced hands at an appropriately equipped center. The vascular ring surgery survival rate at high-volume pediatric centers is among the highest of any congenital anomaly correction, and the long-term outcomes for both quality of life and respiratory function are excellent.
The danger of not operating? For symptomatic patients, the progressive airway damage, recurrent infections, impaired development, and risk of acute decompensation from an untreated vascular ring represent a danger profile that is both more certain and ultimately less manageable than the risks of surgery itself.
FAQs
Q1.Is vascular ring surgery open-heart surgery?
Ans: No, vascular ring surgery is usually not open-heart surgery. It is typically performed through the chest to relieve pressure on the airway and esophagus.
Q2. Is a vascular ring rare?
Ans: Yes, vascular rings are considered rare congenital vascular abnormalities. They occur in a small percentage of children with heart or vascular defects.
Q3. Is a vascular ring congenital?
Ans: Yes, vascular rings are congenital, meaning they are present at birth. They develop during fetal growth when the aortic arch forms abnormally.
Q4. How long does vascular ring surgery take?
Ans: Vascular ring surgery typically takes about 2 to 4 hours, depending on the type and complexity of the vascular ring. Recovery time may vary for each patient.