Intermittent cardiac arrhythmias are among the most diagnostically elusive conditions in medicine. They strike without warning, often resolve within seconds, and leave behind no trace on a standard 12-lead ECG. Over decades, cardiac monitoring technology has evolved in response, from the bulky Holter monitor of the 1960s to modern Event Monitors to today’s sophisticated Mobile Cardiac Telemetry (MCT) systems that transmit data in real time over cellular networks.
Yet despite these advances, a persistent question lingers in both clinical hallways and patient waiting rooms: Should I use Mobile Cardiac Telemetry or an Event Monitor? The answer isn’t always obvious, and choosing the wrong device can mean delayed diagnosis, missed life-threatening arrhythmias, or unnecessary cost.
Understanding the Core Difference
Continuous Intelligence vs Patient-Triggered Recording
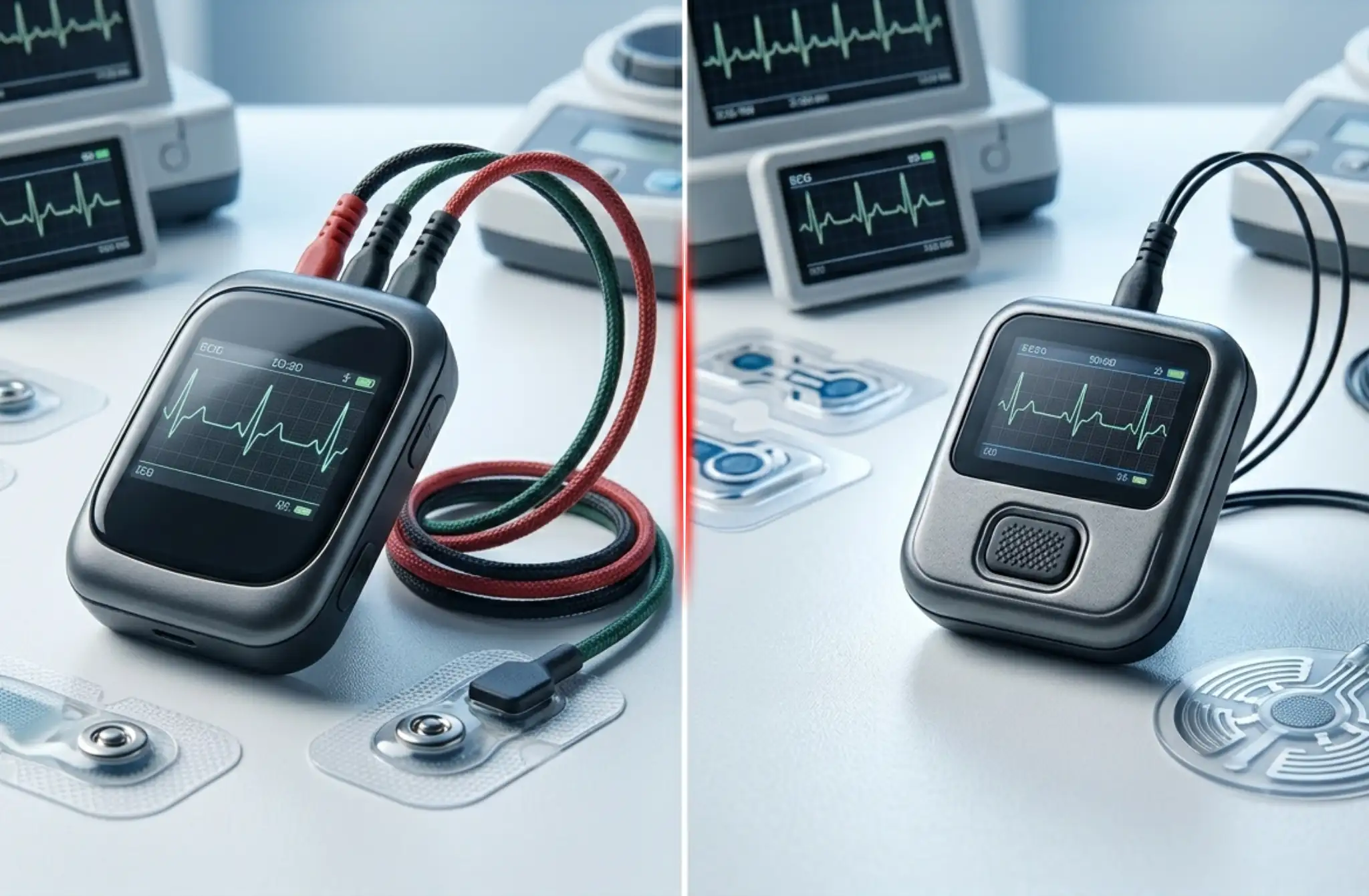
At the heart of this comparison lies a fundamental architectural difference in how each device approaches the problem of capturing a fleeting arrhythmia.
| Mobile Cardiac Telemetry (MCT) ✔Continuous, uninterrupted ECG monitoring ✔Automatic arrhythmia detection algorithms ✔Real-time cellular data transmission ✔24/7 monitoring center oversight | Event Monitor ●Records only when triggered ●Patient activates during symptoms ●Limited auto-trigger in advanced models ●Data reviewed after the fact |
The critical distinction can be distilled into one phrase: MCT is proactive and real-time; Event Monitors are reactive and episodic. This leads directly to the central clinical metric that will appear throughout this guide: diagnostic yield, the percentage of monitored patients in whom a clinically significant arrhythmia is ultimately identified. A high diagnostic yield means fewer repeat tests, faster treatment decisions, and better patient outcomes.
How Mobile Cardiac Telemetry Works
Mobile Cardiac Telemetry represents the pinnacle of current ambulatory cardiac monitoring technology. Unlike its predecessors, MCT doesn’t wait for a patient to push a button; it watches constantly.
How MCT Captures and Transmits Data
1. Wearable electrodes record a continuous ECG signal typically for 14 to 30 days.
2. Onboard AI and algorithmic filters automatically identify abnormal rhythm patterns.
3. Flagged events are transmitted in real time via cellular network to a remote monitoring center.
4. Trained cardiac technicians review incoming data 24 hours a day, 7 days a week.
5. Critical arrhythmias trigger immediate alerts to the prescribing physician or emergency services.
Key Advantages of MCT
✔Detects asymptomatic arrhythmias that the patient never feels, including silent atrial fibrillation
✔Enables immediate clinical response to life-threatening events such as ventricular tachycardia
✔Significantly reduces preventable hospitalizations and ER visits
✔AI-assisted detection reduces human error and improves consistency
Limitations of MCT
- Higher upfront cost compared to traditional monitors
- Requires reliable cellular network coverage throughout the monitoring period
- Generates large volumes of data requiring a robust clinical infrastructure for review
How Event Monitors Work
Event monitors have been a clinical staple for decades. Their design philosophy is elegantly simple: capture an ECG snapshot precisely when the patient feels something wrong. Modern evolution has introduced several variations on this core concept.
| Looping Memory Monitor Continuously records a short loop of ECG data (typically 30–60 seconds). When triggered, it saves the loop plus post-event data, capturing rhythm both before and during symptoms. | Symptom-Triggered Monitor Records only after the patient presses a button. Simpler and cheaper, but entirely dependent on the patient recognizing and responding to symptoms in time. | Auto-Trigger (Hybrid) Monitor Combines patient activation with algorithmic auto-detection. A step toward MCT functionality at a lower cost, but still falls short of true continuous monitoring. |
Key Advantages of Event Monitors
✔Significantly more cost-effective, making them accessible to a broader patient population
✔Well-suited for patients with infrequent but symptomatic arrhythmia episodes
✔Can be worn for extended periods, 30 days or longer, increasing the chances of capturing rare events
Limitations of Event Monitors
- Cannot detect silent or asymptomatic arrhythmias, a critical clinical blind spot
- Heavily dependent on patient compliance and correct triggering behavior
- No real-time alert capability, physician review is passive and delayed
Side-by-Side Comparison
The following table distills the technical and clinical differences into a quick-reference format.
| Feature | Mobile Cardiac Telemetry | Event Monitor |
| Monitoring Type | Continuous (24/7) | Intermittent / Episodic |
| Data Transmission | Real-time cellular | Delayed or manual |
| Arrhythmia Detection | Automatic + AI-assisted | Manual / Limited auto |
| Emergency Alerts | Yes, immediate | Rarely available |
| Best For | High-risk patients | Low-frequency symptoms |
| Diagnostic Yield | High (industry-leading) | Moderate |
| Wear Duration | 14–30 days | Up to 30+ days |
| Cost | Higher | Lower |
| Silent AFib Detection | Yes | No |
| Physician Involvement | Active, real-time monitoring | Passive, retrospective review |
Which Is More Accurate?
Accuracy in cardiac monitoring must be carefully distinguished from detection rate; they are related but not identical concepts.
Accuracy refers to the fidelity of the ECG signal and the correctness of arrhythmia identification. Both MCT and Event Monitors, when properly applied, can produce high-quality ECG recordings. Detection rate, however, measures what proportion of actual arrhythmias the device captures during the monitoring period, and here, the gap between MCT and Event Monitors is substantial.
MCT Excels At Detecting:
✔Silent atrial fibrillation (no symptoms)
✔Nocturnal arrhythmias during sleep
✔Brief, self-terminating episodes
✔High-frequency, unpredictable arrhythmias
Event Monitor Accuracy Depends On:
✔Patient recognizing symptoms accurately
✔Activating the device in time during an episode
✔Symptom frequency during the wear period
✔Consistent wearing and compliance behavior
Clinical Scenarios: When to Use Each
The strongest clinical decisions are guided not by a device’s specifications sheet, but by the patient’s risk profile, symptom pattern, and urgency of diagnosis.
| Use MCT When… ✔Unexplained syncope (fainting) without a clear cause ✔Suspected or confirmed atrial fibrillation ✔Post-stroke cardiac monitoring ✔High-risk patients with prior cardiac events ✔Frequent but unpredictable, potentially asymptomatic arrhythmias ✔Patients who cannot reliably self-monitor | Use Event Monitor When… ●Infrequent, well-recognized palpitations ●Low-risk patients with mild or benign symptoms ●Follow-up monitoring after successful treatment ●Patients who are highly compliant and symptom-aware ●Budget-constrained situations where asymptomatic arrhythmias are unlikely |
Technology Evolution: Where Cardiac Monitoring Is Heading
Cardiac monitoring technology is advancing at a pace that would have seemed science fiction just a decade ago. Several converging trends are reshaping the field:
- AI & Machine Learning Integration:
Deep learning algorithms are achieving cardiologist-level accuracy in arrhythmia classification, dramatically reducing false positives and enabling faster alert generation. - Remote Patient Monitoring (RPM):
MCT is increasingly embedded within broader RPM ecosystems that monitor blood pressure, oxygen saturation, and activity levels alongside cardiac rhythm. - Wearable Tech Convergence:
Consumer devices like smartwatches are beginning to detect atrial fibrillation with clinically meaningful accuracy, blurring the line between consumer health tracking and medical-grade monitoring. - Predictive Analytics :
Next-generation systems are moving beyond detection toward prediction, identifying patients at risk of an arrhythmia event before it occurs.
Common Mistakes When Choosing Between MCT and Event Monitor
Even experienced clinicians fall into predictable traps when selecting cardiac monitoring modalities. Here are the five most critical errors to avoid:
1. Choosing Based on Cost Alone
Budget is a legitimate constraint, but selecting a monitor solely on price without considering diagnostic needs can result in missed diagnoses, repeat testing, and ultimately higher total expenditure.
2. Ignoring Symptom Frequency Patterns
A patient who experiences palpitations three times per day is a different clinical case than one who faints once every three months. Matching monitoring intensity to symptom pattern is fundamental.
3. Underestimating Asymptomatic Arrhythmias
Silent atrial fibrillation is not a rare edge case — it is a leading undiagnosed cause of cryptogenic stroke. Any device incapable of detecting asymptomatic events carries inherent blind spots in high-risk populations.
4. Overestimating Patient Compliance
Clinicians often assume patients will use Event Monitors correctly. In practice, triggering rates are frequently suboptimal. Factor in patient age, cognitive status, and health literacy when selecting device type.
5. Prescribing Without Physician Oversight Planning
An MCT device feeding data to a monitoring center without a clear escalation and alert-response protocol is a liability, not an asset. Infrastructure must match technology.
Conclusion
Choosing between Mobile Cardiac Telemetry and an Event Monitor ultimately comes down to one critical factor: how urgently and accurately an arrhythmia needs to be detected. While Event Monitors remain a practical and cost-effective solution for low-risk patients with predictable, symptom-driven episodes, they fall short in capturing silent or rapidly occurring cardiac events.
Mobile Cardiac Telemetry, on the other hand, represents a more advanced, proactive approach. Learn more about advanced cardiac monitoring solutions and expert care by visiting Atlantic CardioVascular and taking the next step toward better heart health.
FAQS
Q1. Can I shower or bathe while wearing a cardiac monitor?
Most modern monitors are water-resistant but not fully waterproof. You may need to remove or protect the device while showering, depending on the model.
Q2. Do mobile cardiac telemetry devices interfere with daily activities?
No, MCT devices are designed to be lightweight and wearable, allowing patients to continue most normal daily activities, including work and light exercise.
Q3. What happens if a device malfunctions during the monitoring period?
If a device stops working or loses connectivity, patients are usually instructed to contact the provider immediately for troubleshooting or replacement to avoid data gaps.
Q4. Are cardiac monitoring results covered by insurance?
In many cases, insurance covers both MCT and event monitors when medically necessary, but coverage varies depending on the provider and the patient’s condition.
Q5. Can I travel while using a cardiac monitor?
Yes, but with MCT, consistent cellular connectivity is important. Travel to areas with poor network coverage may affect real-time data transmission.