When doctors find a blockage in the coronary arteries, they must determine whether it significantly restricts blood flow. A wrong decision could mean unnecessary procedures or missing a serious risk like a heart attack. In the past, doctors relied on angiography images, but visual assessment alone can be misleading.
To improve accuracy, advanced tests like FFR and iFR were developed to measure actual blood flow using pressure-sensing technology. While both serve the same purpose, they work differently and can impact patient experience and outcomes. Understanding these tests helps patients make more informed decisions about their heart health.
What Is Fractional Flow Reserve (FFR)?
Fractional Flow Reserve, or FFR, is considered the historical gold standard for physiological assessment of coronary artery stenosis. Introduced in the 1990s by Dr. Nico Pijls, FFR fundamentally changed how cardiologists decide whether a blockage needs treatment.
How FFR Works
During an FFR test, a cardiologist inserts a thin, specialized pressure wire through the blockage in the coronary artery. The key step is that the patient is then given a drug called adenosine either intravenously or directly into the artery, which causes the small blood vessels (microvascular bed) to dilate maximally, simulating the conditions of intense physical exercise or stress. This state is called hyperemia.
Why FFR Became the Gold Standard
The landmark FAME and FAME 2 trials firmly established FFR’s clinical utility. The FAME trial demonstrated that FFR-guided stenting reduced the composite of death, heart attack, and repeat revascularization at one year compared to angiography-guided stenting. When doctors find a blockage in the coronary arteries, they must determine whether it significantly restricts blood flow. A wrong decision could mean unnecessary procedures or missing a serious risk like a heart attack. In the past, doctors relied on angiography images, but visual assessment alone can be misleading.
Limitations of FFR
- Adenosine causes uncomfortable side effects, including chest tightness, flushing, breathlessness, and an unpleasant sense of impending doom, although these pass within seconds.
- Adenosine is contraindicated in patients with asthma, certain heart rhythm disorders (AV block), and significant hypotension.
- The drug costs money and adds time to the procedure.
- The requirement for maximal hyperemia means there is a small window of discordance in certain patient populations, such as those with microvascular disease.
What Is Instantaneous Wave-Free Ratio (iFR)?
Instantaneous Wave-Free Ratio (iFR) is a newer physiological test that was designed to provide the same clinical information as FFR but without the need for adenosine or any other drug.
The Science Behind iFR
iFR is built on a key physiological insight: during a specific window of the cardiac cycle called the diastolic wave-free period, the competing forces (pressure waves) that normally affect coronary blood flow are naturally quiescent. During this brief resting window, the relationship between pressure and flow is linear, meaning you can calculate a reliable pressure ratio without artificially creating hyperemia.
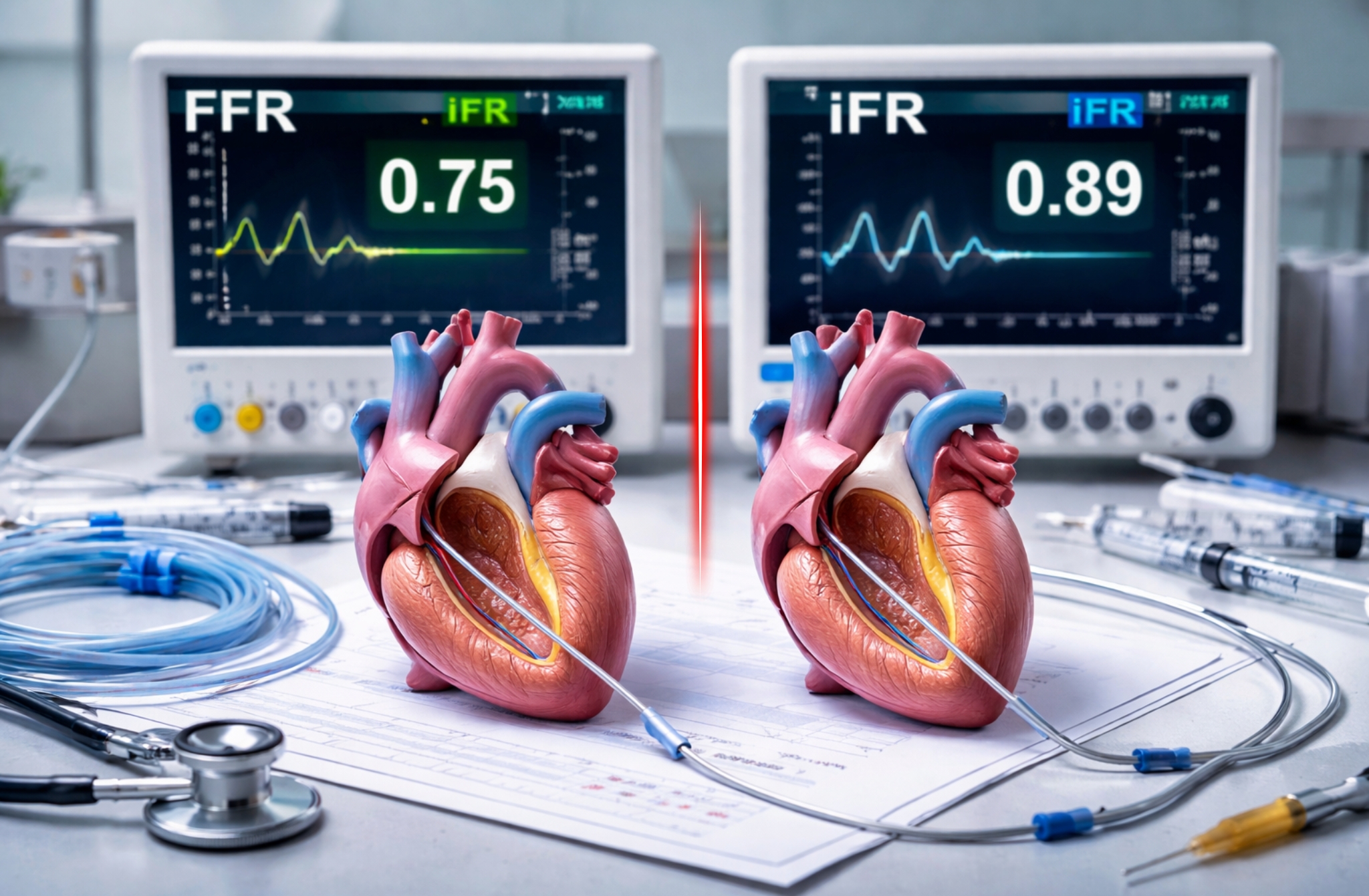
Using the same pressure wire as FFR, iFR measures the ratio of distal coronary artery pressure (Pd) to aortic pressure (Pa) during this specific rest-based diastolic window. The result is averaged across five heartbeats for accuracy. An iFR value of 0.89 or below indicates significant flow restriction requiring treatment.
The Hybrid iFR–FFR Approach
- When doctors find a blockage in the coronary arteries, they must determine whether it significantly restricts blood flow.
- A wrong decision could lead to unnecessary procedures or missing a serious risk like a heart attack.
- In the past, doctors relied on angiography images, but visual assessment alone can be misleading.
- Advanced tests like FFR and iFR were developed to measure actual blood flow using pressure-sensing technology.
- Both tests serve the same purpose but work differently, affecting patient experience and outcomes.
- Understanding these tests helps patients make more informed decisions about their heart health.
FFR vs iFR: Head-to-Head Comparison
The table below summarizes the key differences and similarities between FFR and iFR across the dimensions that matter most clinically and from the patient’s perspective.
| Feature | FFR | iFR |
| Drug Required | Yes (adenosine) | No |
| Measurement Timing | During hyperemia | During diastole (rest) |
| Cut-off Value | ≤ 0.80 = significant | ≤ 0.89 = significant |
| Patient Comfort | Moderate (side effects) | High (no side effects) |
| Procedure Time | Longer | Shorter |
| Cost | Higher | Lower |
| Clinical Accuracy | Gold standard | Equivalent to FFR |
| ACC/AHA Guideline | Class I recommendation | Class IA recommendation |
| Use in ACS | Yes | Limited |
| 5-Year MACE Rate | ~19.9% | ~21.5% (non-inferior) |
The Patient Experience: Comfort and Convenience
Beyond clinical outcomes, the patient experience is a significant differentiating factor between FFR and iFR, and it strongly favors iFR.
Adenosine: The FFR Factor
To achieve maximal hyperemia during FFR, most patients receive intravenous adenosine, typically at doses of 140 mcg/kg/min. The drug works rapidly, but its effects, while short-lived, are frequently distressing. Patients commonly report:
- A tight, crushing sensation in the chest
- Sudden difficulty breathing or shortness of breath
- Facial flushing and warmth
- A disturbing feeling of impending doom or intense anxiety
- Occasional dizziness, nausea, or headache
While these effects resolve within 60–90 seconds of stopping the adenosine infusion, they are unpleasant enough that some patients are reluctant to undergo the procedure. In patients with reactive airway disease (asthma), significant bronchospasm, or hemodynamic instability, adenosine is contraindicated, making FFR inapplicable for a meaningful subgroup.
iFR: A Drug-Free Alternative
iFR requires no pharmacological agents. The patient simply lies still while the measurement is taken during the natural diastolic phase of their heartbeat. Research suggests that iFR can reduce patient discomfort by up to 95.7% compared to FFR. The test is also faster — while adding an FFR evaluation to an iFR assessment adds roughly 10–15 minutes, iFR alone is significantly quicker to perform.
For patients who are already anxious about cardiac catheterization, the removal of adenosine from the equation represents a meaningful quality-of-life improvement.
Cost, Efficiency, and Healthcare Economics
Cost & Savings
iFR reduces per-case costs by eliminating adenosine, which adds drug cost, IV prep, monitoring, and longer procedure time.
Early adoption of FFR already cut costs by reducing unnecessary stenting and readmissions; iFR builds on these savings.
Efficiency
iFR as a first-line assessment speeds up cath lab procedures and increases overall throughput.
Faster procedures lower per-patient costs and improve lab efficiency.
Accessibility
iFR’s drug-free design is especially valuable in lower-resource settings.
Avoids barriers caused by adenosine cost and limited availability.
When Is FFR Used vs When Is iFR Preferred?
Despite iFR’s advantages, FFR remains indispensable in certain clinical situations. The right test depends on patient factors, lesion characteristics, and the clinical question being asked.
When Doctors Prefer FFR
- Acute Coronary Syndrome (ACS): iFR has not been validated for use in acute ST-elevation MI or in the context of active ACS, where microvascular resistance is altered. FFR remains the preferred physiological tool in these scenarios.
- Multivessel CAD with complex anatomy: In complex cases, especially those where the choice between PCI and bypass surgery (CABG) is being weighed, FFR has more extensive trial data, including the FAME 3 trial.
- Grey zone iFR results (0.86–0.93): When iFR falls in the intermediate range, FFR is used as a confirmatory test in the hybrid approach.
- Academic or research settings: FFR has been the standard measurement in the majority of landmark trials, making it preferred in protocols designed around existing evidence.
When iFR Is the Better Choice
- Stable coronary artery disease with intermediate lesions: iFR’s evidence base is strongest for patients with stable angina and moderate stenosis (40–80% narrowing on angiography) exactly the most common diagnostic dilemma.
- Patients who cannot tolerate adenosine: Asthmatics, patients with AV block, or those with hemodynamic instability are better assessed with iFR.
- Multiple vessel assessment: Because iFR is quicker and requires no drug, assessing multiple vessels in a single cath lab session is more practical.
- Patient preference for comfort: For anxious patients or those with a history of poor adenosine tolerance, iFR is the kinder option.
- Resource-constrained settings: Where adenosine supply or IV infrastructure is limited, iFR offers physiological assessment without compromise.
What Do the Cardiology Guidelines Recommend?
Both FFR and iFR carry top-tier endorsements from the world’s leading cardiovascular organizations:
- American College of Cardiology (ACC): Both FFR and iFR carry Class I guideline recommendations for guiding revascularization in intermediate coronary stenosis.
- American Heart Association (AHA): Supports the use of physiological assessment, including both FFR and iFR, in patients with stable ischemic heart disease.
- European Society of Cardiology (ESC): The 2019 ESC Guidelines on Chronic Coronary Syndromes recommend both FFR and iFR with Class IA evidence for assessing the functional significance of lesions.
- Society for Cardiovascular Angiography & Interventions (SCAI): Endorses iFR as a validated physiological tool alongside FFR.
Notably, iFR holds a Class IA recommendation, the highest possible from the ACC, AHA, SCAI, and ESC. This is a distinction that reflects not just the clinical evidence but the strength and consistency of that evidence across multiple major randomized trials and large-scale registries.
So, Which Test Is Better?
The honest, evidence-based answer is that neither test is universally superior; they are tools, and the best tool depends on the clinical context. However, practical considerations are shifting the balance.
The trajectory of clinical practice is clear. As the iFR-SWEDEHEART 5-year data and the 42,000-patient registry analysis have demonstrated, iFR’s non-inferiority to FFR is robust and durable over time. Many leading cardiac centers now use iFR as the default first-line physiological assessment and reserve FFR for specific indications.
The ideal approach for many patients may be the hybrid strategy: start with iFR for its speed and comfort, and step up to FFR only when iFR results are inconclusive. This workflow combines the best of both technologies.
Conclusion
Both FFR and iFR are valuable tools for assessing coronary artery blockages, each with distinct advantages depending on the patient and clinical scenario. iFR offers a faster, drug-free, and more comfortable experience, while FFR remains essential for acute coronary syndromes, complex lesions, or confirmatory testing. For more information on these tests, visit the Atlantic Cardiovascular
For patients and healthcare providers alike, understanding the strengths of each test enables smarter, safer decision-making. These insights can help you make informed choices about your heart health and treatment options.